Diastasis rectus abdominis (or DRA) is a condition that occurs when the tissue between the “6-pack” muscle (the rectus abdominis) thins out due to an increase in abdominal pressure. This increase in pressure can be from a pregnancy, poor breathing strategies, heavy weight lifting with poor strategies, or increased visceral or abdominal fat.
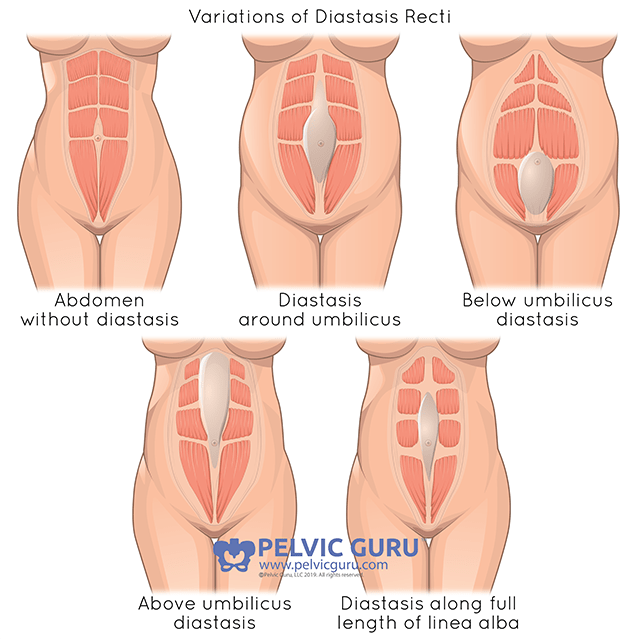
This separation can look different person to person – for some it may just be at the belly button, others it may be above or below the belly button, and others it may be the entire length of the abdominal wall. People will also experience different widths and depths of their diastasis.
The great news is that DRA can be treated, and you can get back to doing what you love with the proper guidance!
There are A LOT of myths surrounding diastasis, which leads to unnecessary hopelessness. So let’s bust some of those myths, shall we??
Myth #1: My abdominal tissue is torn!
Nope! With a diastasis, the tissue is not torn, just stretched out and thinned.The protrusion or depression that some people will see with a diastasis is due to improper activation of the abdominal muscles and poor support of the abdominal wall – not because there has been a tear in the muscle or any of the surround tissues!
This is GREAT news because abdominal muscle can be retrained and strengthened, which is why this condition is treatable!
Myth #2: I need to get the width of my diastasis back to normal.
Actually, you don’t! Research has shown that the width of the diastasis is not indicative of how the abdominal muscles are functioning – crazy right?? However, the DEPTH of the diastasis does provide indicators of function.
Studies have shown that if a diastasis is shallow, the abdominal muscles are supporting the abdominal wall appropriately, even if there are still several finger widths of separation between the rectus abdominis muscle.
If the diastasis has significant depth to it, those deep core muscles (this includes your pelvic floor!) are not supporting your body appropriately and may be weak, tight, and/or poorly coordinated.
Most people do want the width of their diastasis to improve, and for some people it will, others it will not. BUT, what is important to note is that even if the width stays the same, as long as the diastasis is shallow and the depth of it is addressed, the muscles are working appropriately to support your abdominal wall and trunk.
Myth #3: I should avoid all core exercises because it will make my diastasis worse.
NO, NO, and NO.
The key is not avoiding the exercise; it is making sure your body is supporting you appropriately.
This means making sure your deep core muscles are activating well and that you are using good breathing and pressure management strategies so that your abdominal wall is fully supported.
Some basic principles to start with when adding core exercises back into your exercise regime are:
- Avoid breath holding. For most people, exhaling on exertion is easiest.
- Perform exercises with slow, controlled movement. Do not rush.
- If you start feeling symptomatic, stop. This is your body telling you that this exercise may be too much too soon. You’ll get there, just give your body time where it needs it!
- Keep your core engaged to protect your spine and stabilize your pelvis
This is why seeing a pelvic floor PT is so important when returning to exercise postpartum or with a diastasis in general. We can assess your diastasis, determine how well your abdominal wall is being supported, and provide you with the strategies you need to safely exercise!
Onward & Upward,
Allison
